How does RPM billing work for providers?
In 2026, CMS expanded the RPM code set to provide greater clinical flexibility. Providers can now choose between codes based on the amount of data collected and the time spent on management.
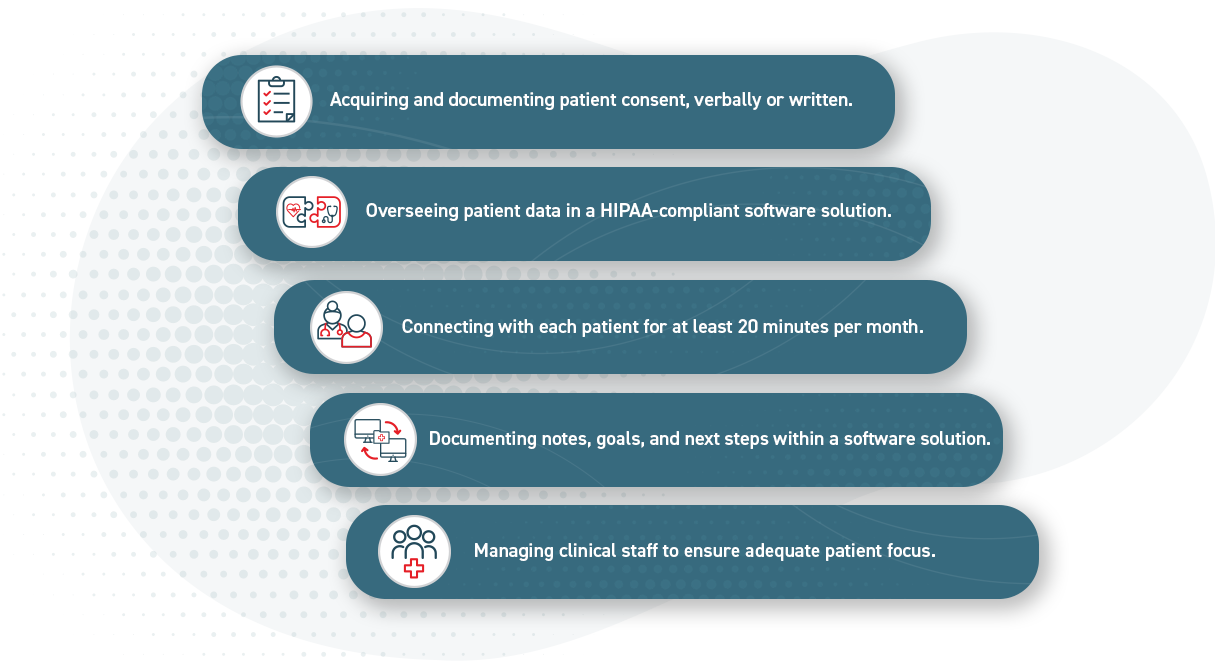
Initial setup and education
- 99453: A one-time code for the initial setup and patient education on how to use the device. Effective 2026, the initial setup code can be billed once a patient has transmitted at least 2 days of data, aligning with the new requirements for acute and episodic monitoring. Rate: $21.71
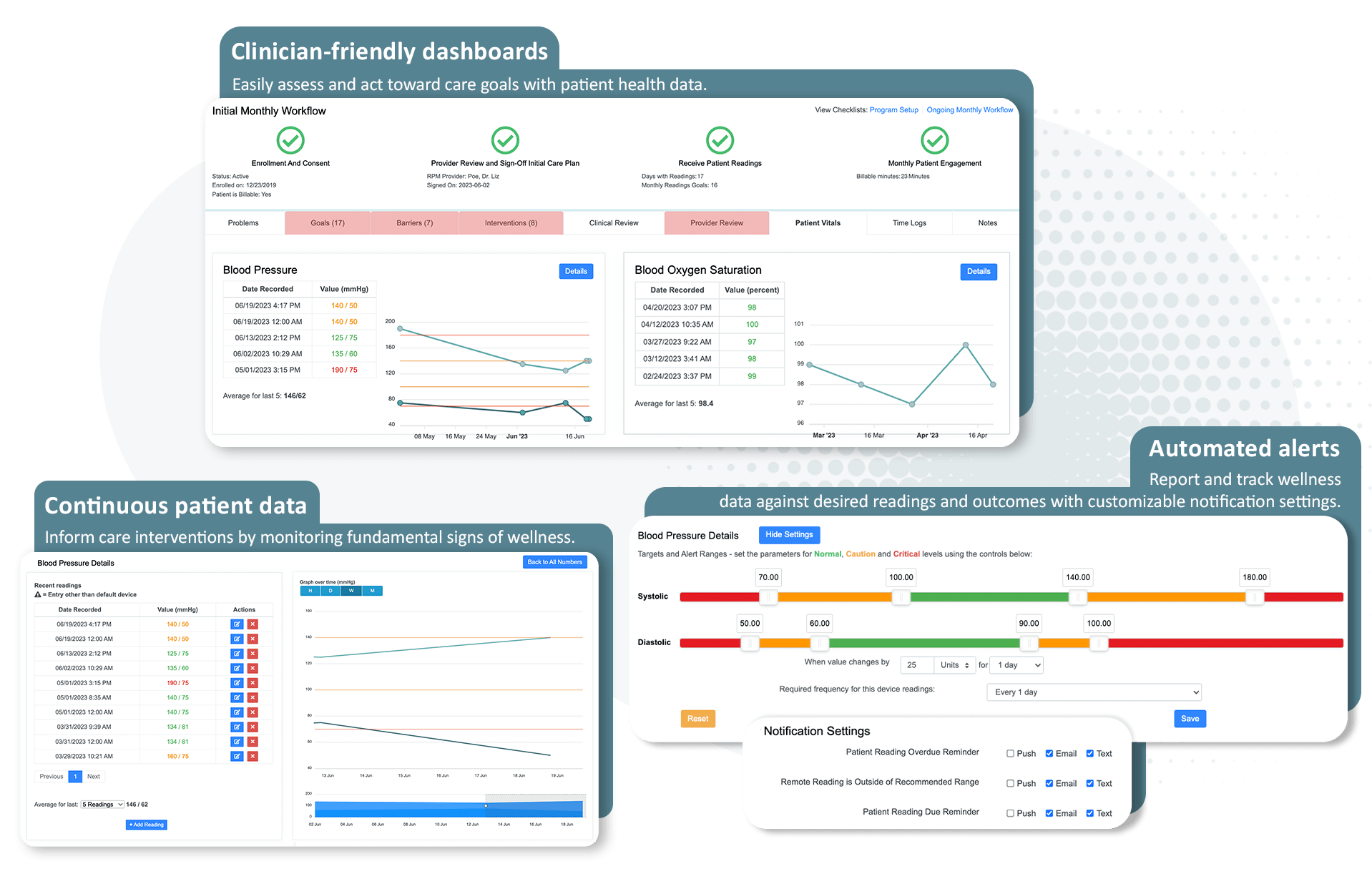
Device supply and data transmission
You must choose one of these codes per 30-day period based on how many days the patient transmitted data. They are not additive.
- CPT 99445 (New): Short-Window Monitoring
- Data Requirement: 2–15 Days of readings
- 2026 National Average: $52.11
- CPT 99454: Standard Monitoring
- Data Requirement: 16–30 Days of readings
- 2026 National Average: $52.11
Strategic Insight: CMS has valued 99445 at the same rate as 99454. This means you no longer lose reimbursement if a patient fails to reach the 16-day threshold, provided they hit at least 2 days of transmission.
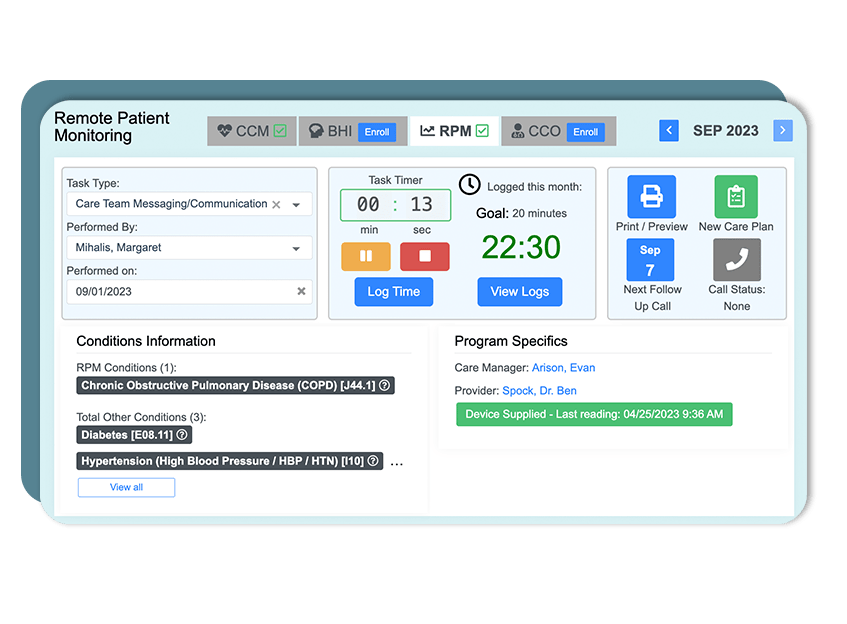
Care management services
These codes cover the time your clinical staff spends reviewing data and interacting with the patient. Choose the code that matches your cumulative monthly time.
- 99470 (New | 10–19 Minutes): Use this for acute check-ins. Requires at least one interactive communication. Rate: $26.05
- 99457 (20 Minutes): The standard monthly management code. Requires at least one interactive communication. Rate: $51.77
- 99458 (Add-on): Each additional 20 minutes of management time beyond the initial 20. Rate: $41.42
Best practices for 2026 compliance
To ensure audit-readiness and maximize ROI, follow these three rules:
- The "Non-Additive" Rule: You cannot bill 99445 and 99454 in the same month. Your software should automatically detect which threshold was met on day 30 and assign the correct code.
- Interactive Communication: Both 99470 and 99457 require at least one real-time interactive communication (phone call or video) with the patient or caregiver per month.
- FDA Compliance: Devices must be FDA-cleared and capable of automatic data transmission. Manual entry (e.g., a patient texting a photo of their scale) does not qualify for reimbursement.






-min%20(1).jpg?width=8659&height=5773&name=iStock-823884700-WWS-PhysicanGroups-1%20(1)-min%20(1).jpg)